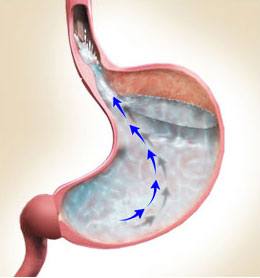
Dyspepsia
Dyspepsia is one of the commonest gastrointestinal (GI) and overall symptoms in general practice. It is defined as a chronic and recurrent pain or discomfort in the epigastrium; often associated with early satiety, post prandial fullness, heartburn and regurgitation. The differential diagnosis includes direct GI pathology such as gastro-oesophageal reflux disease (GORD), peptic ulcer disease, gastric cancer, gastritis and functional causes. Other causes include cholelithiasis, liver pathology and non-abdominal causes such as respiratory and cardiac causes.
Approach
The assessment includes history and examination and may incorporate blood assays, H. Pylori testing and endoscopy. Lifestyle modification advice and empiric therapy using a short course (2 weeks) of proton pump inhibitor is acceptable in the absence of alarm features. In the event of symptom recurrence or in association with alarm features, the gold standard of investigation is upper GI endoscopy.
Alarm features
- Gastrointestinal bleeding/anaemia
- Unintentional weight loss
- Dysphagia or vomiting
- Epigastric mass on palpation
- Family history or high risk for GI cancer
- Previous gastric ulcer or gastric surgery
- Known Barrett’s oesophagus/atrophic gastritis
Endoscopy & H. Pylori
The age limit for endoscopy varies, with 55 years suggested in Western cohorts, whereas 45 years in studies from the East and in our Australian Asian patients. Since H. Pylori was isolated in 1983, it has been implicated in leading to chronic inflammation and metaplasia (ref 1). Testing for H. Pylori includes non-invasive and invasive tests (at endoscopy).
Gastric Cancer
Gastric cancer (GCA) incidence is very low in younger patients with only dyspepsia and no alarm symptoms (0.3% of patients <55 years with GCA only presented with dyspepsia and no alarm symptoms in a multicenter UK trial Ref2) Despite this low incidence, early detection and treatment offers the best outcomes for patients, as demonstrated in a local study of 174 consecutive resections for gastric cancer at Bankstown-Lidcombe Hospital, with the overall 5 year disease free survival at 91% for stage 1 dropping to 39% for stage 3Ref3.
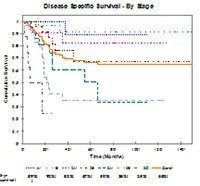
GCA survival graph (ref 3)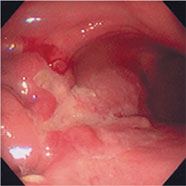
GCA at endoscopy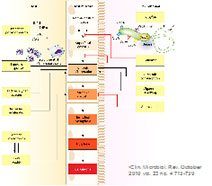
H.Pylori and dysplasia
Gastric Cancer Staging
Current staging mandates the following:
- Chest and abdominal imaging usually with high definition CT scan
- Endoscopic Ultrasound to asses the depth of the lesion and regional nodes (T&N stage)
- Metabolic assessment using FDG PET scan
Adjuvant therapy
Depending on
- Proximity of the tumour to the gastro-oesophageal junction
- Depth of extension (T stage)
- Lymph node involvement (N stage)
Decision is made in the multi disciplinary forum regarding neo adjuvant chemotherapy
Surgical resection
- Open or laparoscopic resection
- Radical total or subtotal gastrectomy
Palliative options
- Local ablative techniques to reduce bleeding
- Self expanding metal stents for obstruction
SYNOPSIS
- The majority of patients presenting with dyspepsia will respond to conservative measures.
- Patients over 45 years, with alarm features or relapsing symptoms should undergo endoscopy.
- Gastric adenocarcinoma works up and management is multimodal and multidisciplinary
- Diagnosis at an early stage infers improved outcomes in patients with gastric cancer














